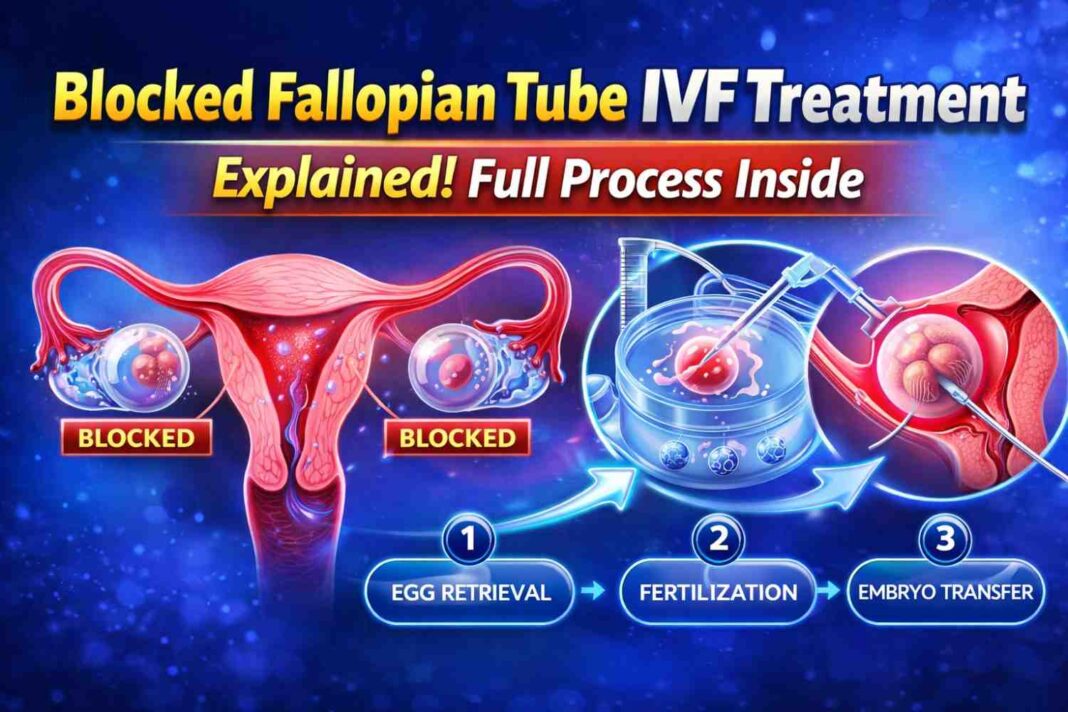
Blocked Fallopian Tube IVF Treatment: When you first hear the words “blocked fallopian tubes,” it can feel like a heavy door has just slammed shut on your dreams of starting a family. I’ve spoken with many women who describe that moment as a mix of confusion and deep frustration—after all, if the “bridge” between the egg and sperm is broken, how can life possibly begin?
The good news is that medical science has a very effective detour. This article is for anyone who has been diagnosed with tubal factor infertility and is wondering if In Vitro Fertilization (IVF) is truly the right next step. We’ll look at why it works, the common hurdles like hydrosalpinx, and a practical workflow to help you move from diagnosis to a positive pregnancy test.
Read This Also: PCOS IVF Treatment Success Tips, Risks & Real Truth Explained
Why IVF is the “Gold Standard” for Blocked Tubes
In a natural conception, the fallopian tube is the meeting point where fertilization happens. If the tubes are blocked due to past infections (like PID), endometriosis, or previous surgeries, the egg and sperm simply can’t find each other.
IVF changes the game by making the fallopian tubes irrelevant.
Instead of relying on the tubes, a fertility specialist collects mature eggs directly from your ovaries, fertilizes them with sperm in a high-tech laboratory, and then places the resulting embryo directly into your uterus. You are essentially bypassing the broken bridge and taking a flight straight to your destination.
The “Hydrosalpinx” Factor: A Critical First Step
One of the most common real-world issues we see is a condition called hydrosalpinx. This is when a blocked tube doesn’t just sit there—it fills with a toxic fluid.
From my experience observing clinical outcomes, this fluid can actually leak back into the uterus. This is a problem because the fluid is “embryo-toxic,” meaning it can wash away an embryo or prevent it from sticking to the uterine wall.
Treatment Options Table: Pre-IVF Prep
Before starting your IVF cycle, your doctor might suggest one of the following to improve your success rates:
| Procedure | What happens? | Why do it? |
| Salpingectomy | Surgical removal of the affected tube. | The “gold standard” to stop toxic fluid leakage and double IVF success rates. |
| Salpingostomy | Creating a new opening in the tube. | Often a temporary fix; fluid can return, but it preserves the physical tube. |
| Tubal Ligation | Tying or clipping the tube near the uterus. | Prevents fluid from leaking into the womb without removing the entire tube. |
| Sclerotherapy | Draining the fluid and “sealing” the tube. | A less invasive, ultrasound-guided option for those avoiding surgery. |
Read This Also: Realme P4 Lite 5G Launched! Biggest Battery Phone Under ₹15K
Your IVF Journey: Step-by-Step Workflow
If you’ve decided to move forward with IVF, here is the routine you can expect. Most cycles take about 6 to 8 weeks from the first injection to the pregnancy test.
1. Ovarian Stimulation: The ovarian stimulation procedure takes about 10-14 days. During this procedure, you’ll be required to take hormone injections. The hormone injections help stimulate your ovaries to produce more than one egg instead of the usual one.
2. Monitoring: After the hormone injections, you’ll be required to visit us at the clinic every 2-3 days. We carry out these checkups through ultrasounds. We carry out these checkups to ensure that your follicles are growing at a safe and steady rate.
3. Egg Retrieval: In this process, you’ll be required to undergo a 20-minute procedure. The process takes place while you’re lightly sedated. A small needle is used to “pick up” the eggs from the follicles.
4. The Lab Phase: In this process, the magic begins. In the lab, your eggs are fused with the sperm. In cases where there are male fertility problems, the process used is called ICSI, where a single sperm is injected into the egg.
5. Embryo Transfer: This process, as you might have already guessed, is the easiest A thin catheter is used to place the best embryo into your uterus. It feels much like a regular pap smear.
Real-Life Mistakes: What I Wish Every Patient Knew
-
Mistake 1: Rushing into IVF without checking for fluid. If you have a hydrosalpinx and ignore it, your chance of a successful IVF cycle can drop by nearly 50%. Always ask your doctor: “Are my tubes just blocked, or are they fluid-filled?”
-
Mistake 2: Assuming “Blocked” means “Useless.” If only one tube is blocked, you might still be a candidate for IUI (Intrauterine Insemination). Don’t assume you must do IVF until you’ve had a full Hysterosalpingogram (HSG) test.
-
Mistake 3: Comparing your “Raw Marks” to others. Every woman’s ovarian reserve is different. Focus on the quality of the embryos produced, not just the quantity of eggs retrieved.
Summary: Taking Back Control
A tubal blockage is a mechanical problem, not a sign that you cannot be a mother. IVF is the most direct and successful way to overcome this specific hurdle. By addressing any underlying fluid issues first and following a structured stimulation protocol, most women with blocked tubes see success rates comparable to those with no fertility issues at all.
FAQs:
Q1: What is Blocked Fallopian Tube IVF Treatment?
Blocked Fallopian Tube IVF Treatment is a process where IVF bypasses blocked tubes to achieve fertilization outside the body.
Q2: Can pregnancy happen naturally with blocked tubes?
In most cases, natural pregnancy is not possible if both tubes are blocked, which is why Blocked Fallopian Tube IVF Treatment is recommended.
Q3: How long does IVF treatment take?
Blocked Fallopian Tube IVF Treatment usually takes around 6 to 8 weeks from hormone stimulation to embryo transfer.
Q4: What is hydrosalpinx and why is it treated first?
In Blocked Fallopian Tube IVF Treatment, hydrosalpinx is fluid in the tube that can harm embryo implantation, so it must be treated first.
Q5: What is the success rate of IVF in blocked tubes?
Blocked Fallopian Tube IVF Treatment has a good success rate, especially for women under 35, often around 45–55% per cycle.