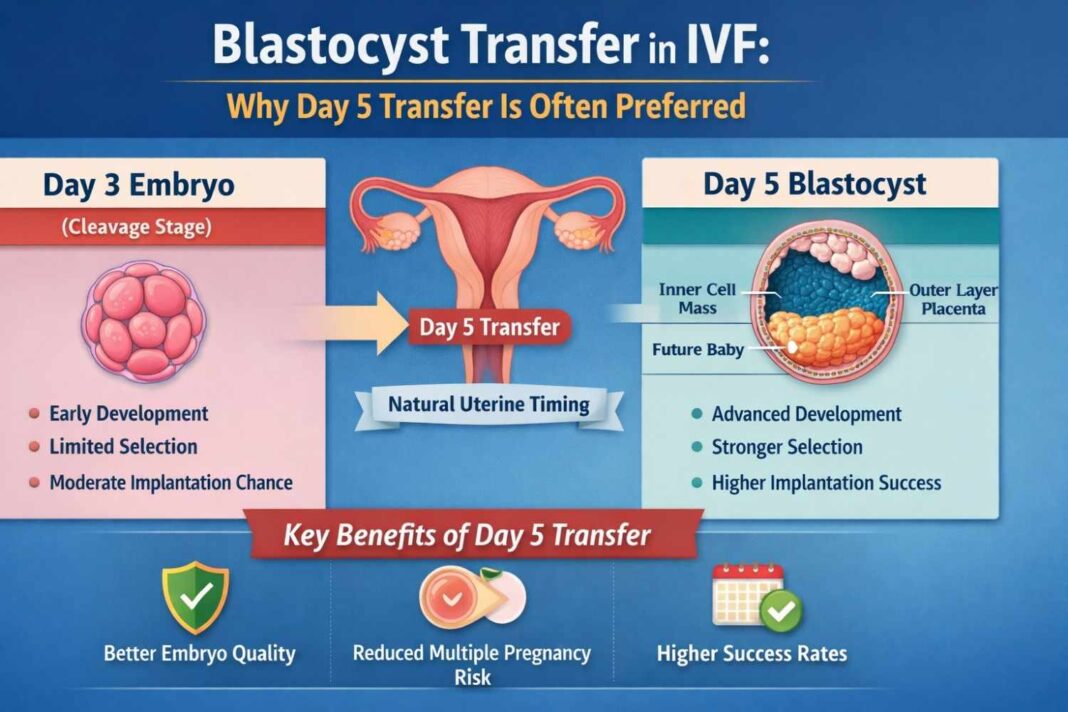
Blastocyst Transfer in IVF: For many couples in India, the US, and the UK, IVF is not just a treatment — it’s an emotional journey filled with decisions that feel overwhelming. One of the biggest decisions during an IVF cycle is whether to proceed with a blastocyst transfer.
I’ve seen patients come into consultations confused about what “blastocyst” even means, and more importantly, whether waiting until Day 5 is truly better than transferring earlier. This article breaks it down clearly, without jargon, so you understand what happens, why clinics recommend it, and what you should realistically expect.
What Is a Blastocyst Transfer?
In IVF, eggs are fertilized in the lab. The resulting embryos grow in a controlled environment.
-
On Day 2–3, embryos are in early stages (cleavage stage).
-
By Day 5 or 6, some embryos develop into a blastocyst.
A blastocyst has:
-
A fluid-filled cavity
-
An inner cell mass (which becomes the baby)
-
An outer layer (which becomes the placenta)
When we transfer a Day 5 embryo into the uterus, that’s called a blastocyst transfer.
Read This Also: IVF with Own Egg vs Donor Egg: Which Option Is Right for You?
From experience, the main reason doctors recommend blastocyst transfer is selection. Not all embryos survive to Day 5. The ones that do tend to be stronger.
Here’s why that matters:
-
Better natural selection
If an embryo can grow to blastocyst stage, it has already passed several developmental checkpoints. -
Improved synchronization
In a natural cycle, embryos reach the uterus around Day 5. A blastocyst transfer better matches that timing. -
Lower risk of multiple pregnancy
Because success rates per embryo are generally higher, clinics often transfer just one blastocyst.
That said, it’s not automatically the right choice for everyone.
Step-by-Step: What Actually Happens in a Blastocyst IVF Cycle
Step 1: Ovarian Stimulation
You take hormone injections for about 8–12 days to stimulate multiple eggs. Regular scans and blood tests monitor growth.
Why it matters: The number and quality of eggs influence how many embryos reach Day 5.
Step 2: Egg Retrieval
A minor procedure under sedation. Eggs are collected using ultrasound guidance.
Recovery is usually quick — mild cramping for a day or two.
Step 3: Fertilization
Eggs are fertilized either by standard IVF or ICSI (where a single sperm is injected).
Embryos are monitored daily.
Step 4: Extended Culture to Day 5
Instead of transferring on Day 3, embryos stay in the lab longer.
This is the critical waiting period. Some embryos stop developing — and that’s completely normal.
Common mistake: Patients assume losing embryos before Day 5 means failure. In reality, those embryos likely would not have implanted.
Read This Also: India Women vs Australia Women 2026 – Adelaide Thriller Full Highlights
Step 5: Blastocyst Transfer
The procedure itself is simple and usually painless. No anesthesia needed.
A thin catheter is used to place the embryo into the uterus under ultrasound guidance.
You rest briefly, then go home.
Blastocyst vs Day 3 Transfer: A Practical Comparison
| Factor | Day 3 Transfer | Blastocyst (Day 5) Transfer |
|---|---|---|
| Embryo stage | Early | More developed |
| Selection strength | Limited | Stronger natural selection |
| Implantation potential | Moderate | Often higher per embryo |
| Risk if few embryos | Safer option | Risk of having none to transfer |
| Common use today | Less common | Increasingly preferred |
If you have very few embryos, some doctors may recommend Day 3 transfer to avoid the risk of having none survive to Day 5.
Who Is a Good Candidate for Blastocyst Transfer?
From clinical observation, it often works well for:
-
Women under 38 with good ovarian response
-
Patients with multiple embryos
-
Those planning single embryo transfer
-
Couples doing genetic testing (PGT)
It may not be ideal if:
-
You produce very few eggs
-
Previous cycles resulted in low embryo survival
Always discuss this based on your individual case — not someone else’s IVF story.
Emotional Reality: The Day 5 Waiting Period
This part isn’t discussed enough.
The extra two days of waiting between Day 3 and Day 5 can feel longer than the stimulation phase. Patients often call the clinic repeatedly, anxious about how many embryos are left.
Here’s what helps:
-
Ask your clinic how often they update patients.
-
Avoid comparing numbers with others.
-
Focus on quality, not just quantity.
Practical Checklist Before Blastocyst Transfer
- Understand how many embryos you have on Day 3
- Discuss the risk of having none reach Day 5
- Clarify if a frozen transfer is planned
- Ask about single vs double embryo transfer
- Review your uterine lining thickness
Having these answers reduces anxiety and avoids last-minute confusion.
Takeaway: Is Blastocyst Transfer Better?
It can be — but only in the right context.
Blastocyst transfer allows better embryo selection and aligns closely with natural implantation timing. However, it’s not a universal solution. The best choice depends on age, egg quality, number of embryos, and previous IVF history.
In my experience, informed patients handle the process better — not because outcomes are guaranteed, but because expectations are realistic.
FAQs About Blastocyst Transfer in IVF
1. Does blastocyst transfer guarantee higher success?
No method guarantees success. It may improve implantation rates per embryo, but overall outcomes depend on multiple factors.
2. What if no embryos reach Day 5?
It can happen, especially with low embryo numbers. This doesn’t mean IVF will never work — adjustments can be made in future cycles.
3. Is the transfer procedure painful?
Most women describe it as similar to a Pap smear — mildly uncomfortable at most.
4. Is bed rest required after transfer?
Extended bed rest is usually unnecessary. Normal light activity is fine unless your doctor advises otherwise.
5. Should I choose fresh or frozen blastocyst transfer?
Both options work. Frozen transfers are increasingly common because they allow better hormonal preparation.
6. How many blastocysts are typically transferred?
In many clinics in India, the US, and the UK, single embryo transfer is recommended to reduce twin risk.